Reflux, heartburn, indigestion, GORD…
These are all names for that awful sensation when acid from your stomach escapes upwards into the oesophagus. For many, this means burning in the lower ribcage and chest, or for those with silent reflux, pain may not occur until the acid reaches the throat.
Reflux can also contribute to nausea, chest pain, difficulty swallowing and shortness of breath.
So, what’s causing all this stomach acid to move up your oesophagus and what can we do about it?
What’s causing it?
All reflux is essentially caused by an opening of the gastroesophageal sphincter (‘the what?’ I hear you ask).
At the point where your stomach meets your oesophagus, there is a small circular muscle, called a sphincter (such a great word). When this muscle contracts, it seals up the stomach and prevents stomach acid flowing back into the oesophagus. If there is an opening at this muscle, then the acid can escape and cause reflux.
There are lots of reasons why this muscle might not be able to close properly including:
1. Weakening of the sphincter muscles
Sometimes the sphincter muscle can become weak, which means that although it’s trying to contract and seal off the stomach, it doesn’t quite close. The poor little guy is doing his best, but he’s just not able to stop the acid sneaking out.
2. Hiatus hernia
This is when the stomach pops through the diaphragm, causing the oesophagus to sit at a weird angle. This can sometimes make it difficult for the sphincter to close properly:
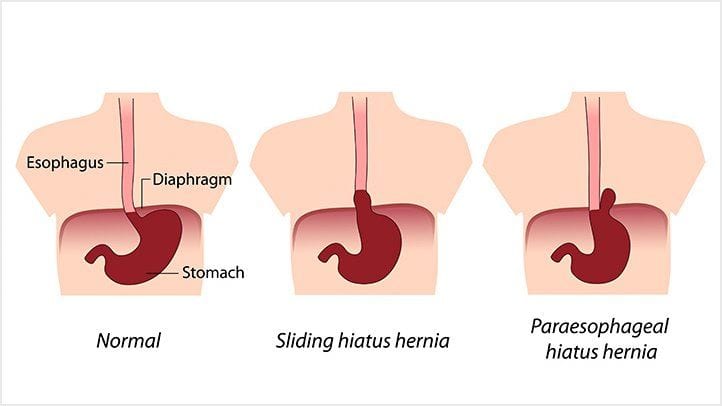
Image source
3. Pregnancy
When you’re growing a human in your lower abdomen, all your other organs just have to make room. This can put upward pressure on your stomach, compressing it into a smaller space and at a different angle to where it normally sits. At this angle the sphincter may not be able to close normally and there is less room in your stomach, making it easier for acid to escape into your oesophagus.
4. Weight gain
As your body weight increases, so does the volume of tissue in your abdomen which puts upward pressure on your stomach. If your sphincter is already weak, this can make symptoms of reflux more frequent and severe.
What can we do about it?
1. Use gravity
In managing reflux, gravity is your friend. When we are sitting or standing upright, gravity helps to keep gastric acid and your food in the lower part of your stomach while it churns and breaks down. However, when you lie down, there is more opportunity for that acid to flow closer to your sphincter and up into the oesophagus.
For this reason, one of the best things you can do to manage reflux is avoid lying down, reclining or going to bed in the hours after a main meal. This can mean having dinner a bit earlier, or choosing a different chair to keep you upright.
You can also consider raising your torso when you do go to bed so that there is some gravitational pull on your stomach contents while you sleep. You can do this by raising the head of the bed 10 -15 cm or buying a wedge to place under the mattress.
Your posture can have a big impact on how much gravity can help reflux. If you’re standing or sitting up straight, your torso is stretched out, giving your stomach a bit more room and allowing gravity to draw acid down, away from the oesophagus. But, if you are hunched over, then your abdominal cavity and your stomach is compressed. Stretches and exercises can help you to improve posture and likely help to manage reflux in the long term.
To limit the impact of posture on reflux, after eating and drinking:
- Try to stretch out your torso and stand/sit up straight.
- Avoid couches and chairs that cause you to slouch
2. Reduce food volume
When you eat a large meal, or a lot of food in a short period of time, you fill your stomach up and the food volume brings gastric acid closer to your sphincter. This is the main reason why small, frequent meals are recommended as a strategy to manage reflux.
But what does small, frequent meals look like? Well, it depends on the individual. We suggest planning for 5- 7 meals throughout the day, giving yourself a few hours in between to allow your stomach to empty. Another suggestion would be to also try and avoid eating 2-3 hours before bed. This is an example of what a day may look like with small frequent meals:
7:00am – Cereal and milk
- ½ cup high fibre cereal
- ½ cup milk
9:00am – Strawberries and nuts
- 1 punnet of strawberries
- ¼ cup mixed nuts
11:00am – Veggies and dip
- 1-2 cups chopped veg
- 2 Tbsp dip
1:00pm – Toasted sandwich
- 2 slices of wholemeal bread
- 2 slices of cheese
- 1 tomato, sliced
- ½ cup baby spinach
3:00pm – Apple and peanut butter
- 1 x apple
- 1 Tbsp peanut butter
5:00pm – Rice cakes with tuna
- 2 rice cakes
- 1 x 90g can flavoured tuna
7:00pm – Stir fry
- 100 -150g pork strips
- ½ cup cooked rice
- 2 cups stir fry veggies
3. Keep an eye on fat & protein volumes
Both protein and fat take longer to digest in your stomach, compared to carbohydrates, fibre and water. This means that protein and fat sit in your stomach for long and require more acid to break them down. All of this extra work simply provides more opportunity for acid to reach your sphincter and travel up your oesophagus.
These meals and foods are particularly high in fat and/or protein and are more likely to cause symptoms of reflux:
Fried foods like:
- Hot chips
- Fried chicken
- Donuts
Pub meals like:
- Chicken schnitzel
- Chicken parmigiana
- Large steak meals
Burgers with chips
Curries with lots of oily or coconut sauces
Large portions of nuts, avocado.
Creamy pasta sauces.
Sausages and salamis
Try to keep an eye on how often these might slip into your week, and whether they contribute to reflux symptoms.
4. Avoid irritants
Irritants are chemicals that stimulate your stomach to churn or produce more acid, which can increase the changes that you will get back flow into the oesophagus. These can be very different depending on the individual, so there is no one-size-fits-all recommendation on what to avoid. If you find that having tomatoes doesn’t contribute to pain or discomfort, you may not need to avoid it to manage your reflux.
However, if you are getting regular symptoms, reducing some of these things can help to ease the severity of your symptoms day-to-day.
Common gastric irritants include:
- Coffee
- Alcohol
- Spicy food
- Acidic foods such as;
Orange juice
Tomatoes
Lemon
Vinegar
5. Medications & Surgery
There are several medications that can be purchased over the counter or prescribed by a doctor to neutralise acid or reduce the production of gastric acid.
There are also surgical measures which can be taken to reduce the size of the hole in your diaphragm, so that your oesophagus closes over more. As with any major surgery there are risks and possible complications.
It’s always best to speak to your doctor about what the right option is for you.
If you want to learn more about how changes to your pattern of eating might help to reduce reflux, then get in contact with our team at The Healthy Eating Clinic.